Whether it’s auto, property, or life insurance, when an unfortunate event happens, the policyholder will request compensation from the insurer based on their policy. This process, through which the insured notifies the insurer and the insurer takes all necessary steps until the policyholder receives compensation, is called the “Insurance Claim”. Many of us have gone through such a process and found it time-consuming, with the insurer requesting various documents, leaving you unsure of how long it will take or how many trips you’ll need to make to the post office or the insurer’s office. Let’s explore how new technologies can improve the process so that the end customer benefits from a better interaction experience with the insurance company.
Hyper-Automating an Insurance Claim Process
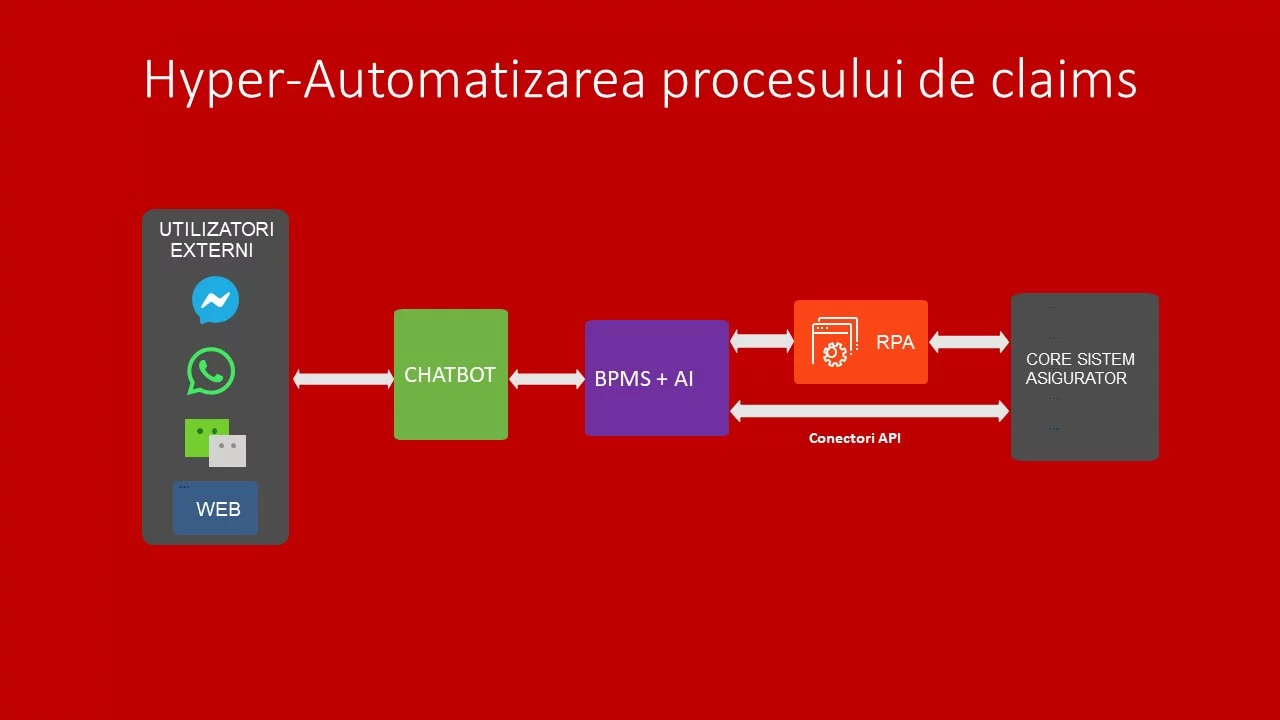
We can almost completely automate a claims process using three types of automation technologies embedded in a unique hyper-automation solution:
- A state-of-the-art chatbot capable of conversing with customers, collecting information from them, and informing them of the steps that need to be followed;
- A low-code BPM platform that allows the definition of all steps in the claims process, the connections between them, and the actions performed by operators;
- An RPA robot capable of automatically operating data in the insurer’s various software applications, relieving human operators from repetitive and time-consuming tasks.
Description of the Claims Process
Event Notification – The first step in the claims process is the notification of the event by the insured. The insured goes to the insurer’s website, Facebook, or WhatsApp and initiates a conversation with an AI-powered chatbot capable of answering all their questions and guiding them in preparing the documents necessary to open the file.
File Opening – In the second step, the information collected and validated by the chatbot is automatically transmitted via API to the BPM platform. This platform initiates the opening of the claim file and, based on the information received, checks in the insurer’s internal systems to see if there are policies related to the insured, if they are active, and if they cover the reported event.
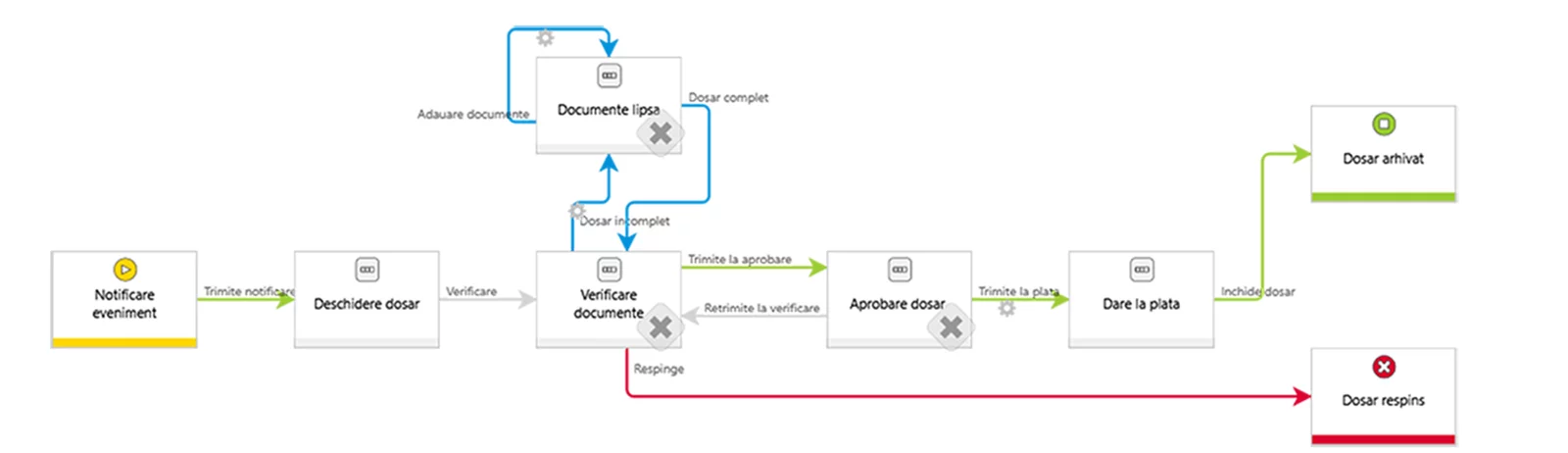
Document Verification – In this step, the BPM system notifies a specialist from the claims department that a new file has been assigned to them. The specialist checks the information and intervenes where necessary, requesting new documents or information from the insured.
File Completion – The chatbot contacts the insured via WhatsApp or Facebook Messenger, informs them of the additional documents required, and provides all the details for obtaining them. When the insured obtains the documents, they upload them from their phone or computer into the chatbot’s dialogue window, which transmits them to the BPM.
File Approval – The claims specialist validates the documents and sends them for approval to a superior. The superior can view and approve them from a laptop or mobile phone. Upon approval, the BPM system generates the payment report.
Payment Processing – An RPA robot processes the payment report in the payment system and other core internal systems. When the payment is successfully processed, the BPM system sends the payment information to the chatbot, which then notifies the client of the amount and account to which the transfer was made and requests feedback from the insured.
File Closure – In the final step of the process, the BPM system records the feedback collected by the chatbot, closes the file, and transfers the necessary data to other internal systems.
What Are the Benefits of an Automated Claims System?
- Increased Customer Satisfaction – The customer receives all necessary information instantly, at any time, via the chatbot. Additionally, the chatbot helps the customer complete the forms;
- Increased Employee Satisfaction – Employees no longer need to process paper documents or incorrectly completed forms, and the BPM brings all necessary information onto a single screen;
- Increased Process Compliance – All operations carried out by robots or humans are automatically recorded for audit purposes;
- Increased Process Efficiency – The claims process is executed faster, with fewer iterations where the customer needs to send documents, fewer errors, and less manual activity;
- Continuous Improvement – AI algorithms will analyse thousands of claim files and recommend further system improvements by identifying areas where it operates slowly, steps where errors occur, elements that are frequently filled out incorrectly by the customer, and the most common questions from policyholders.
